June 2024
Orthotic Devices
 Orthotics are devices inserted into shoes to support, align, or improve the function of the feet. They help relieve pain and prevent injuries by redistributing pressure and providing support to specific areas of the foot. This can alleviate issues such as plantar fasciitis, flat feet, and overpronation, reducing strain on muscles and joints. Although there are various types of orthotics, rigid, semi-rigid, and soft, determining which type works best for an individual's condition can be somewhat unpredictable. The effectiveness of orthotics largely depends on the specific foot problem and the unique biomechanics of the patient. For optimal results, it is suggested that if you are interested in understanding more about orthotics, you schedule an appointment with a podiatrist who can perform a thorough evaluation of your foot condition and overall health and determine if orthotics are right for you.
Orthotics are devices inserted into shoes to support, align, or improve the function of the feet. They help relieve pain and prevent injuries by redistributing pressure and providing support to specific areas of the foot. This can alleviate issues such as plantar fasciitis, flat feet, and overpronation, reducing strain on muscles and joints. Although there are various types of orthotics, rigid, semi-rigid, and soft, determining which type works best for an individual's condition can be somewhat unpredictable. The effectiveness of orthotics largely depends on the specific foot problem and the unique biomechanics of the patient. For optimal results, it is suggested that if you are interested in understanding more about orthotics, you schedule an appointment with a podiatrist who can perform a thorough evaluation of your foot condition and overall health and determine if orthotics are right for you.
If you are having discomfort in your feet and would like to try orthotics, contact Dawn Miles, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Are Orthotics?
Orthotics are inserts you can place into your shoes to help with a variety of foot problems such as flat feet or foot pain. Orthotics provide relief and comfort for minor foot and heel pain but can’t correct serious biomechanical problems in your feet.
Over-the-Counter Inserts
Orthotics come in a wide variety of over-the-counter inserts that are used to treat foot pain, heel pain, and minor problems. For example, arch supports can be inserted into your shoes to help correct overarched or flat feet, while gel insoles are often used because they provide comfort and relief from foot and heel pain by alleviating pressure.
Prescription Orthotics
If over-the-counter inserts don’t work for you or if you have a more severe foot concern, it is possible to have your podiatrist prescribe custom orthotics. These high-quality inserts are designed to treat problems such as abnormal motion, plantar fasciitis, and severe forms of heel pain. They can even be used to help patients suffering from diabetes by treating foot ulcers and painful calluses and are usually molded to your feet individually, which allows them to provide full support and comfort.
If you are experiencing minor to severe foot or heel pain, it’s recommended to speak with your podiatrist about the possibilities of using orthotics. A podiatrist can determine which type of orthotic is right for you and allow you to take the first steps towards being pain-free.
If you have any questions please contact one of our offices located in Palatka and Saint Augustine, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Managing Pain of Diabetic Foot Problems
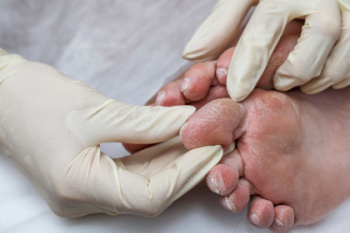 Diabetic foot ulcers and peripheral neuropathy are common complications of diabetes, often resulting in significant pain and discomfort. Neuropathy, caused by prolonged high blood sugar levels, damages the nerves, leading to numbness, tingling, and pain in the feet. Ulcers develop due to reduced blood flow and the inability to sense injuries, allowing minor wounds to progress into serious infections. Assessment involves a thorough examination of the feet, checking for signs of neuropathy, poor circulation, and existing ulcers. Podiatrists use tools like monofilaments to test sensation and Doppler devices to assess blood flow. Management focuses on controlling blood sugar levels, proper wound care, and preventing further complications. Pain from neuropathy is treated with medications, while ulcers require cleaning, debridement, and specialized dressings. Custom orthotics and appropriate footwear can alleviate pressure on affected areas. If you suffer from diabetic-related foot problems, it is suggested that you are under the care of a podiatrist for optimal care.
Diabetic foot ulcers and peripheral neuropathy are common complications of diabetes, often resulting in significant pain and discomfort. Neuropathy, caused by prolonged high blood sugar levels, damages the nerves, leading to numbness, tingling, and pain in the feet. Ulcers develop due to reduced blood flow and the inability to sense injuries, allowing minor wounds to progress into serious infections. Assessment involves a thorough examination of the feet, checking for signs of neuropathy, poor circulation, and existing ulcers. Podiatrists use tools like monofilaments to test sensation and Doppler devices to assess blood flow. Management focuses on controlling blood sugar levels, proper wound care, and preventing further complications. Pain from neuropathy is treated with medications, while ulcers require cleaning, debridement, and specialized dressings. Custom orthotics and appropriate footwear can alleviate pressure on affected areas. If you suffer from diabetic-related foot problems, it is suggested that you are under the care of a podiatrist for optimal care.
Wound care is an important part in dealing with diabetes. If you have diabetes and a foot wound or would like more information about wound care for diabetics, consult with Dawn Miles, DPM from Florida. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
What Is Wound Care?
Wound care is the practice of taking proper care of a wound. This can range from the smallest to the largest of wounds. While everyone can benefit from proper wound care, it is much more important for diabetics. Diabetics often suffer from poor blood circulation which causes wounds to heal much slower than they would in a non-diabetic.
What Is the Importance of Wound Care?
While it may not seem apparent with small ulcers on the foot, for diabetics, any size ulcer can become infected. Diabetics often also suffer from neuropathy, or nerve loss. This means they might not even feel when they have an ulcer on their foot. If the wound becomes severely infected, amputation may be necessary. Therefore, it is of the upmost importance to properly care for any and all foot wounds.
How to Care for Wounds
The best way to care for foot wounds is to prevent them. For diabetics, this means daily inspections of the feet for any signs of abnormalities or ulcers. It is also recommended to see a podiatrist several times a year for a foot inspection. If you do have an ulcer, run the wound under water to clear dirt from the wound; then apply antibiotic ointment to the wound and cover with a bandage. Bandages should be changed daily and keeping pressure off the wound is smart. It is advised to see a podiatrist, who can keep an eye on it.
If you have any questions, please feel free to contact one of our offices located in Palatka and Saint Augustine, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Blisters Caused by Edema
 Edema, which is caused by excess fluid retention in the body, can also result in the development of blisters on the feet. These blisters are caused by the swelling that occurs when fluid collects in the tissues, causing pressure to be put on the skin. The skin then becomes more susceptible to friction and rubbing, especially in areas where it makes contact with shoes or socks. The increased friction can cause the formation of blisters, which can lead to pain and discomfort. Blisters caused by edema mainly appear on the feet and ankles, making daily activities like walking and wearing shoes difficult and painful. It is important to address the underlying cause of edema to prevent the formation of blisters. A podiatrist can provide personalized treatment options to manage edema and alleviate foot discomfort. Recommendations include compression socks or orthotic inserts to reduce swelling and friction. If you are developing blisters caused by edema, it is suggested that you visit a podiatrist for an exam and appropriate treatment options.
Edema, which is caused by excess fluid retention in the body, can also result in the development of blisters on the feet. These blisters are caused by the swelling that occurs when fluid collects in the tissues, causing pressure to be put on the skin. The skin then becomes more susceptible to friction and rubbing, especially in areas where it makes contact with shoes or socks. The increased friction can cause the formation of blisters, which can lead to pain and discomfort. Blisters caused by edema mainly appear on the feet and ankles, making daily activities like walking and wearing shoes difficult and painful. It is important to address the underlying cause of edema to prevent the formation of blisters. A podiatrist can provide personalized treatment options to manage edema and alleviate foot discomfort. Recommendations include compression socks or orthotic inserts to reduce swelling and friction. If you are developing blisters caused by edema, it is suggested that you visit a podiatrist for an exam and appropriate treatment options.
Blisters are prone to making everyday activities extremely uncomfortable. If your feet are hurting, contact Dawn Miles, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters develop as a result of constantly wearing tight or ill-fitting footwear. This happens due to the constant rubbing from the shoe, which can often lead to pain.
What Are Foot Blisters?
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
How Do Blisters Form?
Blisters on the feet are often the result of constant friction of skin and material, usually by shoe rubbing. Walking in sandals, boots, or shoes that don’t fit properly for long periods of time can result in a blister. Having consistent foot moisture and humidity can easily lead to blister formation.
Prevention & Treatment
It is important to properly care for the affected area in order to prevent infection and ease the pain. Do not lance the blister and use a Band-Aid to provide pain relief. Also, be sure to keep your feet dry and wear proper fitting shoes. If you see blood or pus in a blister, seek assistance from a podiatrist.
If you have any questions, please feel free to contact one of our offices located in Palatka and Saint Augustine, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Understanding Ankle Sprains and Strains

Ankle sprains and strains are injuries that can significantly impact your mobility and daily activities. A sprain occurs when the ligaments, which are the tough bands of tissue connecting bones at the ankle joint, are abnormally stretched or torn. Conversely, a strain involves similar damage but affects muscles or tendons, which are the tissues that connect muscles to ankle bones. These injuries can result from repetitive motions or a sudden incident, like a twist or fall. Diagnosis by a podiatrist typically involves a medical history review and physical examination, and may include imaging tests, such as X-rays, CT scans, or MRIs. While most sprains and strains heal over time with rest, bracing, and anti-inflammatory medications, more severe cases may require surgery for a full recovery. It is important to manage these injuries properly to prevent chronic pain or instability. If you experience an ankle sprain or strain, it is suggested that you contact a podiatrist who can provide an accurate diagnosis, tailored treatment plan, and guidance on rehabilitation exercises.
Although ankle sprains are common, they aren’t always minor injuries. If you need your ankle injury looked at, contact Dawn Miles, DPM from Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains are the result of a tear in the ligaments within the ankle. These injuries may happen when you make a rapid shifting movement while your foot is planted. A less common way to sprain your ankle is when your ankle rolls inward while your foot turns outward.
What Are the Symptoms?
- Pain at the sight of the tear
- Bruising/Swelling
- Ankle area is tender to touch
- In severe cases, may hear/feel something tear
- Skin discoloration
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
In many cases, the RICE method (Rest, Ice, Compression, and Elevate) is used to treat ankle sprains. However, you should see a podiatrist to see which treatment option would work best with your injury. In severe cases, surgery may be required.
It is important to ask your doctor about rehab options after you receive treatment for your injury. Stretching, strength training, and balance exercises may help the ankle heal while also preventing further injury.
If you have any questions, please feel free to contact one of our offices located in Palatka and Saint Augustine, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.